Do I have Plantar Fasciitis?
 If you suffer from 2 or more of the above you likely have Plantar fasciitis
If you suffer from 2 or more of the above you likely have Plantar fasciitis
Pain
I have pain in the heel and or in the arch area.
Difficulty with walking
Pain with putting foot to ground first thing in the morning. Eases in less than 1 hour.
Different footwear or bare feet influence my pain
I find that I need to avoid certain shoes to be more comfortable.
Better with medications or applying ice
I find that I am using ice or medications (analgesics/anti inflammatories)
What is the Plantar Fascia?
The plantar fascia is a thick fibrous connective tissue that spans a large portion of the under the surface of the foot. It runs from the heel to the base of the toes so to provide support the arch of the foot as the tissue undergoes tension when the foot is weight bearing. The plantar fascia also has a role in energy conservation during weight bearing tasks like walking and running. Finally, it also serves as a broad tissue attachment for other muscles in the foot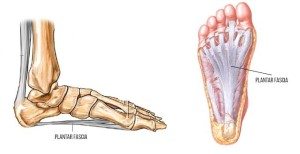
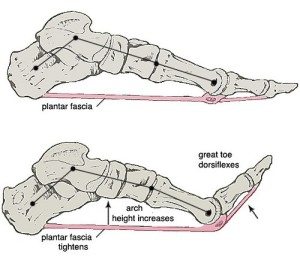
Plantar fasciitis is the most common cause of heel pain and accounts for up to 15% of all foot symptoms among adults. It is classified as an overuse injury, where in this case ‘overuse’ can result from various changes such as:
- Wearing shoes you haven’t worn before or a shoe you haven’t worn in a while i.e. thongs
- Increase in walking or running distance/time/speed
- Changes to your gait pattern i.e. a new running style or limping as a result of another injury
- Changes in the surface area you’re walking or exercising on
Plantar fasciitis has more recently been likened to other tendon related overuse injuries, despite not being a tendon. This similarity has been drawn due to a similar structure and function. These injuries occur over time as we continue to load these tissues without allowing for adequate rest and recovery time between bouts of exercise, or if the exercise intensity/duration is too greater increase. Over time the structural make-up of the plantar fascia changes and as a result, the ability of the tissue to absorb load reduces and subsequent pain instills.
What are the symptoms of a Plantar Fasciitis?
In most cases, plantar fasciitis presents as a gradual onset of the heel or plantar foot pain that is generally worse during the first steps in the morning or after periods of inactivity. The pain tends to improve with activity throughout the day and then worsens towards the end of the day with increased weight-bearing tasks, though this presentation can vary throughout cases.
What causes plantar fasciitis?
Plantar fasciitis is defined as an overuse injury (Lemont et al., 2003). Prior to the onset of symptoms increased amount of weight-bearing activity, such as walking and running, can cause an overuse response within the plantar fascia that progresses to generate degenerative changes causing the symptoms of plantar fasciitis. Overuse can come in many forms, not just increased load-bearing activity, and in the case of plantar fasciitis changes in footwear or exercise surface can alter the dynamics of plantar foot tissue, enough to generate an overuse response (Cole, Seto, & Gazewood, 2005).
Differential Diagnosis:
Imaging is limited in its ability to diagnose plantar fasciitis though it may be utilised in order to rule out other possible conditions. Calcaneal stress fractures and other bony lesions can mimic the clinical symptoms of plantar fasciitis and may require MR imaging or a bone scan to be ruled out.
A tear of the plantar fascia can present with similar symptoms however the onset of pain is resultant of a mechanism or sudden onset and may cause an inability to weight-bear after the initial injury and with other physical activity.
Tarsal tunnel syndrome or compression of the medial calcaneal branch of the posterior tibial nerve can cause symptoms of heel and plantar foot pain, though the type of pain is usually of a burning nature. Symptoms involving neurological tissue may also present with pain that radiates up the leg. There will also be notable tenderness over the medial aspect of the heel or inferior to the medial part of the ankle.
Treatment
Mainstay
The mainstay treatments with greatest supporting evidence for treatment of plantar fasciitis revolve around re-training and improving load-absorbing properties of the plantar fascia. This is mainly achieved with a structured progressive exercise program that may progress to impact weight bearing tasks such as running and jumping depending on each individual’s goals.
There is also evidence to support load altering strategies such as the use of orthotics, changing footwear or taping strategies. Essentially identifying the cause of overuse and altering physical load can have a strong influence on pain reduction.
ADJUNCT THERAPIES
As research is done over a population of people with a condition, some people may respond to treatments that others don’t, however when analysing the research as a whole it may suggest these therapies to be ineffective, though a more statement would be that they can be effective for some people but not all.
Some strategies that are cost effective and have some efficacy in treating plantar fasciitis include:
- Use of ice, or specifically in plantar fasciitis freezing a water bottle and rolling it under the foot
- Massage
- Anti-inflammatory medication
- Stretching
It is important to note that the changes these treatments make are often short-term and can be well used along with mainstay treatments, however are likely not to lead to resolution when used on their own.
In cases where conservative management fails, a corticosteroid injection may be appropriate, but is still coupled with exercise and load management strategies. In rare cases where all management fails over long periods, surgical intervention may be required.
When can I return to activity
01
Your Physiotherapist will advise you as to when you are safe to return to sport/activity.
02
You can speed things up by an accurate rehabilitation program. Your Physiotherapist will provide you with exercsies and a management plan.
03
If you do not have a Physiotherapist download a program below and contact uswith any questions you may have?
How do I make an appointment?
Select from the page menu your closet Physica Clinic. We look forward to you attending.
5 Hot Tips for fixing your plantar fasciitis
· Avoid wearing flat shoes or walking in bare feet
· Regular stretching of the plantar surface of the foot, particularly when getting out of bed and after inactivity
· Reduce painful weight-bearing tasks for a period of 2 weeks
· Adopt other exercises such as swimming or bike riding as a replacement for running until the pain settles.
Ensure you have a shoe assessment to check that you are wearing the correct shoes for your activity. Your Physiotherapist can assist with this.
· Utilising a frozen water bottle as a roller for the under surface of your foot at the end of the day
References
Alshami, A. M., Souvlis, T., & Coppieters, M. W. (2008). A review of plantar heel pain of neural origin: differential diagnosis and management. Manual Therapy, 13(2), 103-111. doi:10.1016/j.math.2007.01.014
Buchbinder, R. (2004). Plantar Fasciitis. The New England Journal of Medicine, 350(21), 2159-2166. doi:10.1056/NEJMcp032745
Cole, C., Seto, C., & Gazewood, J. (2005). Plantar fasciitis: evidence-based review of diagnosis and therapy. Am Fam Physician, 72(11), 2237-42.
Lemont, H., Ammirati, K. M., & Usen, N. (2003). Plantar Fasciitis: A Degenerative Process (Fasciosis) Without Inflammation. Journal of the American Podiatric Medical Association, 93(3), 234-237. doi:10.1.1.624.9029
Neufeld, S. K., & Cerrato, R. (2008). Plantar fasciitis: evaluation and treatment. Journal of the American Academy of Orthopaedic Surgeons, 16(6), 338-346.
Rolf, C., Guntner, P., Ericsäter, J., & Turan, I. (1997). Plantar fascia rupture: diagnosis and treatment. The Journal of foot and ankle surgery, 36(2), 112-114.
